Neovascularization: The Growth of New Blood Vessels in the Retina
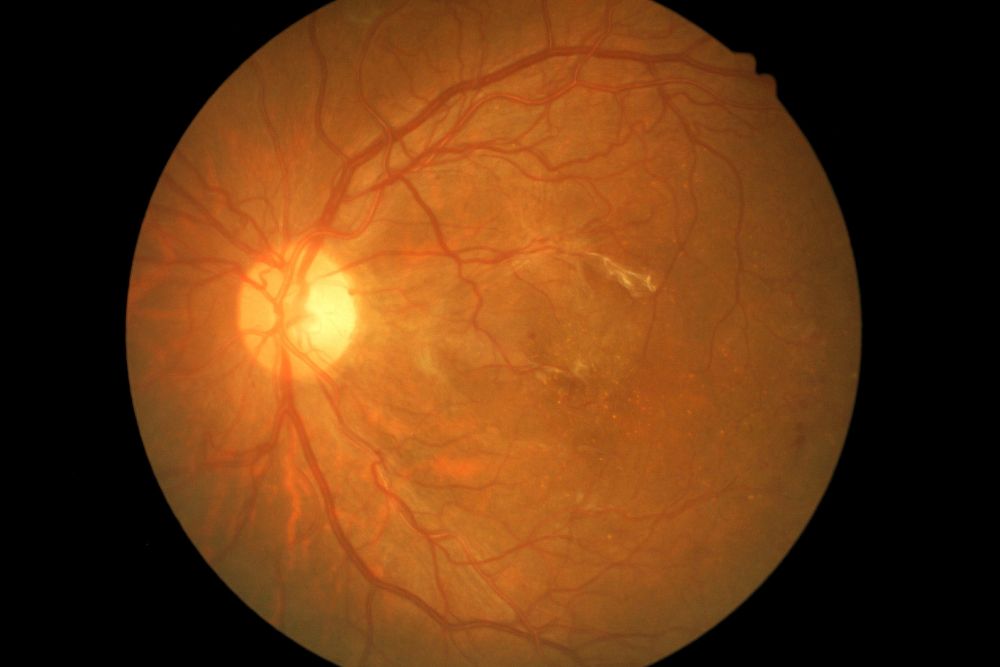
The process of neovascularization involves the growth of new blood vessels to replace those lost due to injuries or conditions. These new vessels easily break, causing fluid and blood to leak into the retina or other parts of the eye, leading to various visual disturbances and issues. Neovascularization is a serious aspect of several retinal conditions and can cause permanent vision loss if not detected, monitored, and treated early on. However, by being vigilant about your vision health and seeing your retina specialist for regular eye exams, you have a much greater chance of reducing the damage done by neovascularization and preserving your vision.
Common Conditions Involving Neovascularization
Wet Age-Related Macular Degeneration (AMD)
The leading cause of irreversible vision impairment among people over 50, age-related macular degeneration (AMD) is a degenerative condition affecting the macula, the retina’s center, which enables central vision and the ability to see in fine detail. AMD starts out as dry AMD, in which the macular cells gradually deteriorate. For about 10% of patients with AMD, the disease progresses into a more advanced form known as wet AMD. The hallmark of wet AMD is choroidal neovascularization (CNV), which affects the choroid – a spongy, pigmented layer of blood vessels and connective tissue that supplies the retina’s outer layers with oxygen and blood. As vessels break, blood and other fluids leak into the macula, causing symptoms like central vision blurriness and vision loss.
Diabetic Retinopathy
A complication of diabetes, diabetic retinopathy is a progressive condition that involves high blood sugar levels weakening the retina’s tiny blood vessels. The most advanced form of the condition, known as proliferative diabetic retinopathy (PDR), is characterized primarily by the presence of neovascularization. As fluid seeps under the macula, the risk of developing a vision-threatening condition, such as retinal detachment, increases. In some cases, significant vision loss and permanent blindness can occur. Diabetic macular edema may also develop, in which fluid or blood builds up and causes the macula to swell.
Retinal Vascular Occlusions
The retina is supported by a complex network of blood vessels, including a central artery that supplies the retina with freshly oxygenated blood and a central vein that directs depleted blood away from the retina and back to the heart for recirculation. The retinal vascular system also includes many small branches of blood vessels that originate from the central artery and vein. Just like any other blood vessel in the body, the retinal central artery, central vein, and their related branches can be obstructed or blocked off, also known as occlusion. Retinal vascular occlusions disrupt the eye’s normal blood cycle; neovascularization occurs as an attempt to remedy the problem and restore normal vascular function. However, because the new blood vessels are abnormal and fragile, they only make things worse, causing a wide range of vision problems.
Neovascularization Treatment Options
Treating neovascularization typically depends on the specific cause, however, the primary treatment method is intravitreal injections of vascular endothelial growth factor (anti-VEGF) medications. These medications work by inhibiting the proteins responsible for new blood vessel growth, thereby stopping the abnormal blood vessels from forming.
Laser treatment may also be employed to close off leaky blood vessels or stabilize the retina. These techniques include photodynamic therapy, which combines light and light-sensitive medications to close damaged blood vessels, and panretinal photocoagulation.
Learn How Neovascularization Affects Retinal Function
For disorders involving abnormal blood vessel growth, understanding the retinal impact allows you to recognize symptoms, permitting earlier diagnosis and treatment. If you’d like to request an appointment with a retina specialist in the Central Savannah River Area, please contact The Retina Eye Center today.
